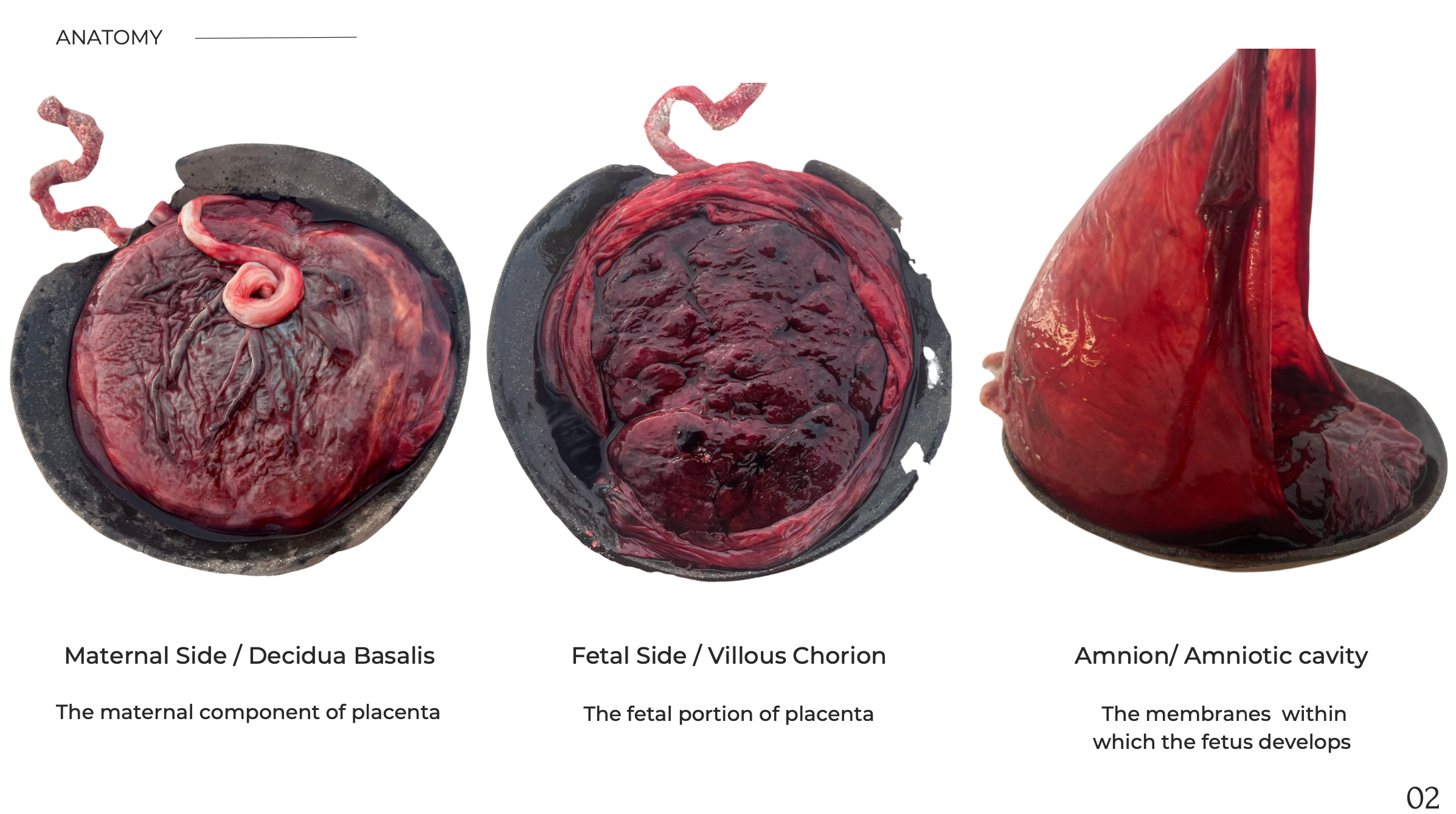
The Placenta is the origin of every human being
-Bailey Sonora
During pregnancy and after birth, the placenta makes maternal and child survival possible
How can a vital organ that carries significant weight by making life possible, be disregarded as medical and spiritual waste? Respect shown to the placenta is ancient, cultures throughout the world hold significant meaning to the attribution of the placenta, and how the placenta is a spiritual anchor for the newborn child to live a healthy and wholesome life. The majority of postpartum hemorrhage is associated with the state and/or retention of the placenta after birth. It is important to recognize and understand the physical and spiritual embodiment of the placenta in pregnancy and birthing. -
Cultures throughout the world recognize the symbol of the tree of life within the placenta. The tree of life represents the living embodiment of humans connection and place within the natural world. The umbilical cord is a spiritual time-keeper, in the beginning of conception the placenta is formed to sustain new life and the umbilical cord is our connection to the sustenance of our mothers and this earth as human beings. The umbilical cord is a continuing of time in the life cycles of birth and death. The planting of placenta, places humans within the natural world in a way that roots them into place and time within the continuation of creation. There are countless stories of human beings originating from each continent who care for the placenta is unique ways such as; burial, drying, wrapping in grasses to be hung in a tree, consuming through food as medicine, and preservation. All to honor the second born soul of the child and connect this child to the earth through ceremonial and honorable handling.
-
Delayed cord clamping is the prolongation of the time between the delivery of a newborn and the clamping of the umbilical cord.
“Early” cord clamping is generally carried out in the first 60 seconds after birth (generally within the first 15–30 seconds), whereas “delayed” umbilical cord clamping is carried out more than 1 min after the birth or when cord pulsation has ceased.
Delay of cord clamping allows more blood to transfer from the placenta to the baby, sometimes increasing the child’s blood volume by up to a third. The iron in the blood increases the newborn’s iron storage, which is vital for healthy brain development.
Immediate cord clamping deprives the baby of 30% of the baby’s blood volume which can cause hypovolemia, anemia and the need for blood transfusion.
Delayed cord clamping results in higher hematocrit and hemoglobin levels
Increased iron stores by 6 months in age
More time transitioning to life outside the womb
Increased blood volume for the baby
Decreased chances of anemia in the baby
For the first few minutes after birth, there is still circulation from the placenta to the infant. Waiting to clamp the umbilical cord for 2–3 min, or until cord pulsations cease, allows a physiological transfer of placental blood to the infant (the process referred to as “placental transfusion”), the majority of which occurs within 3 min. This placental transfusion provides sufficient iron reserves for the first 6–8 months of life, preventing or delaying the development of iron deficiency until other interventions.
The latest research suggests that clamping the umbilical cord too early, before “spontaneous respirations” — those first few newborn breaths in about the first 25 seconds of life — can affect cardiovascular changes, not allowing proper dilation of the lungs’ blood vessels before they’ve fully filled to allow the baby to breathe oxygen.
In general, both the American College of Obstetricians and Gynecologists (ACOG) and the American Academy of Pediatricians (AAP) recommend delaying cord clamping for both full-term and pre-term newborns.
-
The placenta is generally considered to be medical waste, and if an individual does not articulate that she wants to keep the placenta, it’s disposed of in accordance with hospital policy. However, some women do want to keep the placenta after birth – there are ample cultural and personal reasons for this.
Most birth centers allow parents to bring their placenta home
Take Home Placenta Checklist;
Agreement from birth center, hospital, and health providers take home your placenta
Support person who will be at the birth to ensure your placenta requests are carried out
Two quart plastic bowls with tight fitting lid, or two large heavy duty ziplock bags
New Mexico requires that free standing birth centers develop policies and procedures for “safe handling of the placenta for families requesting to keep the placenta” permitting its release without a court order.
For hospital births, ask for a consent to release placenta form. Have this document filled out entirely, signed, and ensured it is entered into your OB chart with prior discussion with your provider. Ask what is required to take home the placenta ( Some hospitals require a small ice chest with specific requirements, some will send it home in a biohazard bag, some states require a court ordered release )
Since 2006 a few states have enacted laws protecting a birthing parents access to their placenta. Native Hawaiians are to thank for this, as the state of Hawai'i was the first to require explicitly that allow women or their designees to take their placentas home. Oregon, Hawaii and Texas each have a separate law that allows mothers to take the placenta home. Even in states that do not have these laws, some hospitals let women take the placenta home once they sign a liability waiver.
By federal law, the hospital retains the right to keep a portion of the placenta for any testing if necessary or concern for risk of infectious disease. Provided that a mother fills out a consent to release placenta form requesting the placenta, and then tests negative for certain infectious diseases, she’s free to take it with her upon discharging from the health care facility.
Having a statute on the books doesn’t necessarily mean it will be followed. If a woman wanting to keep her placenta has an emergency delivery involving EMS techs, for example, and the EMS techs dispose of the placenta, there’s no realistic recourse for getting it back even though she had a legal right to retain it.
This speaks to the importance of making one’s wishes known at the outset of having any medical care. When a woman checks into a hospital to give birth, and wants to keep her placenta, she should have the form ready as part of her admission packet, and she should also have it on file with her OB-GYN doctor.
-
Plant at home in a meaningful place, or a place of intention for your child, for example if I want my children to have a relationship with horses I would plant my placenta near the entrance of a horse corral.
Wrap the placenta in grasses, fabric, or herbs to bury with good thoughts for the Childs life.
Dry a section of the umbilical cord for a keepsake.
Put placenta in a clay or meaningful vessel to be be buried in the ground or directly in a vessel. This way it is portable and can be moved if necessary.
Placenta encapsulation as medicine.
Freezing the placenta is an option if an individual is undecided on what they want to do.
-
The regulation for human placenta is intricate and underenforced.
The placenta is an organ though does not meet the federal definition of organs under the National Organ Transplant Act, given that it cannot be used for direct transplantation. Instead, the placenta is regulated as a “Human Cell Tissue Product” which leaves this symbolic and culturally meaningful organ susceptible to mistreatment.
Within the complex cycle of placental economies, some individuals may be in the position to become customers of their own bodies. The buying back of placenta takes several forms, from placenta based drugs, clinical products, cosmetics, skin lotions, and hair treatments.
Beginning in 1959-1990s human placentas were a widespread ingredient in mainstream personal care products and beauty treatments in the United States. Todays mainstream cosmetics are more likely to be sourced from animal placentas, though human placentas continue to be used and manufactured in East Asian countries, particularly Japan and South Korea. These products containing placental hormones are associated with premature sexual development and increased risk of breast cancer due to elevated estrogen exposure.
Publicy traded, for-profit biopharmaceutical companies such as MiMedx for example, market stem-cell therapies, regenerative, and therapeutic applications that utilize human amniotic materials, placental tissue, and umbilical cord tissue.
Manufactuers are not required to disclose ingredients that they consider trade secrets or required to report on past formulations of their products. North American distributor Flawless Beauty and Skin sold human placenta based products in the United States such as Authentic Relumins Advance Whitening Facial Cream. The FDA took Flawless Beauty to the U.S. District Court of New Jersey and was ordered to stop selling, recall, and destroy its placental products. This company still exists today selling products online.
Companies claiming to accept placenta donations that help improve the health and life of others, have been revealed in using placental tissue to manufacture and market lucrative products. The gendering of placental tissue donation is compounded by the fact that it is overwhelmingly men who reap the economic benefits associated with the research, processing, and selling of ideas and products derived from placentas.